Type a search + hit enter!

Extended breastfeeding – or nursing a child beyond the first year of life – is becoming more common in the United States due to public health efforts to normalize breastfeeding and scientific evidence of the benefits of breastfeeding. However, policy and research are only a piece of the puzzle. Social media influencers and bloggers are […]
read more
latest post

read more
Extended breastfeeding – or nursing a child beyond the first year of life – is becoming more common in the United States due to public health efforts to normalize breastfeeding and scientific evidence of the benefits of breastfeeding. However, policy and research are only a piece of the puzzle. Social media influencers and bloggers are also a huge part of the effort to normalize breastfeeding. Rachel, a mother from Michigan (@chasingthechalfants) is one of the people helping to normalize breastfeeding and has shared quite a bit of her parenting journey on Instagram. Recently, we got to interview Rachel about her experience nursing twins for 19 months. Here’s what she had to say:
Hi! My name is Rachel and I’m the face behind @chasingthechalfants on Instagram. I am a former elementary school teacher turned stay-at-home mom to a 4 year old (Landon) and 19 month old twins (Carter and Ella). My husband, 3 kids and I live in Ann Arbor, MI. When I’m not chasing after the kids, I enjoy chugging (too much) iced coffee, cooking, reading and solo trips to Target. My favorite part of being a mom is getting to be there for all the (not so) little moments and seeing their personalities develop and change. Follow along on Instagram for daily shenanigans, cooking, motherhood and more!
-
How did you fuel your body to keep up with feeding twins and has that changed over the 19 months? When the twins were born I was literally nursing around the clock and I was SO hungry. In addition to eating a variety of foods to fuel my body and theirs, I also drank a ton of water. I knew that hydration was so important and continues to be. While there were no particular foods I ate to fuel my body, I tried to eat a balanced diet but also honor any cravings I had. After all, I was feeding two little humans and was running on little sleep. As they’ve gotten older and are now nursing less, I continue to make food choices that I know will fuel me to chase after 3 toddlers. Water is still a huge piece and hydration is so important, whether you’re nursing or not.
-
What did your feeding schedule look like? I nursed on demand and continue to do so. Sometimes that means nursing one at a time and sometimes that means tandem nursing, although that’s gotten more complicated since they’ve gotten older. Thankfully a few nursing essentials made tandem nursing a lot easier – the twin Boppy pillow and the My Brest Friend Twin Pillow. Having a supportive nursing pillow to support both babies made such a huge difference.
-
When you fed at the same time, what positions did you find to work best for you? When they were younger, I always used a nursing pillow (mostly the My Brest Friend Twin pillow) or a pillow under each of them to support their heads. Now that they’re older, they’re in a whole host of positions. We joke that I am like a swim up bar – they’ll both walk up to me, have a seat and nurse! Sometimes, one will lay across my lap and the other will sit in front of me. If it sounds a little crazy, that’s because it is! But it works.
-
Did you ever worry you wouldn’t produce enough milk for both babies? Since their weights dropped significantly below birth weight after we were discharged from the hospital, we started supplementing with formula almost immediately after they were born. This actually took a lot of pressure off of me because I knew they were getting the nutrients they needed and it wasn’t solely dependent on how much milk I was producing. During the first couple months, I would nurse both babies and my husband would supplement with bottles of formula. As they got older, we have had to make a few changes due to bottle strikes, but I have always felt confident that between nursing and bottles (then formula, now whole milk), both babies were getting everything they needed.
-
What resources did you rely on when you were having a tough time breastfeeding? Outside of talking to friends and family, I mostly relied on local Facebook groups for support. We have a great local mom’s Facebook group in our city as well as local parents of multiples group. Both were great in offering support, suggestions, and being able to connect with other twin moms was especially helpful. As with most things, but especially in parenting, simply knowing that you’re not alone or not the first person to experience something is helpful in and of itself. It was also helpful to talk to friends and family who reminded me that they were there for support and that there were other breastfeeding resources available.
-
Moms say that breastfeeding adds another layer to their relationship with their infant. How did breastfeeding affect your relationship with each infant? Not surprisingly, breastfeeding twins feels a lot different than breastfeeding a singleton. In the beginning, I often felt like I was nursing 24/7 (and sometimes I actually was) so I don’t know that the breastfeeding connection was necessarily present then. But now that they’re older and things have slowed down a bit, the times when I’m able to nurse just one baby at a time is so special. As a mom, looking down and making eye contact with a nursing baby is one of the most special feelings in the world. It adds a layer of connection, love, and intimacy that I haven’t felt before. I cherish those quieter moments when I realize just how amazing my body is and what a special bond I have with each of my children.
Thank you so much, Rachel, for sharing your experience! Keep being awesome!

read more
Over the past 10 years we have seen a rise in the number of states where marijuana sales and use are legal. This has opened the door for women to publicly ask about, and for researchers to publicly investigate marijuana use during lactation. There are properties of marijuana that raise concern about it’s use during […]
read more
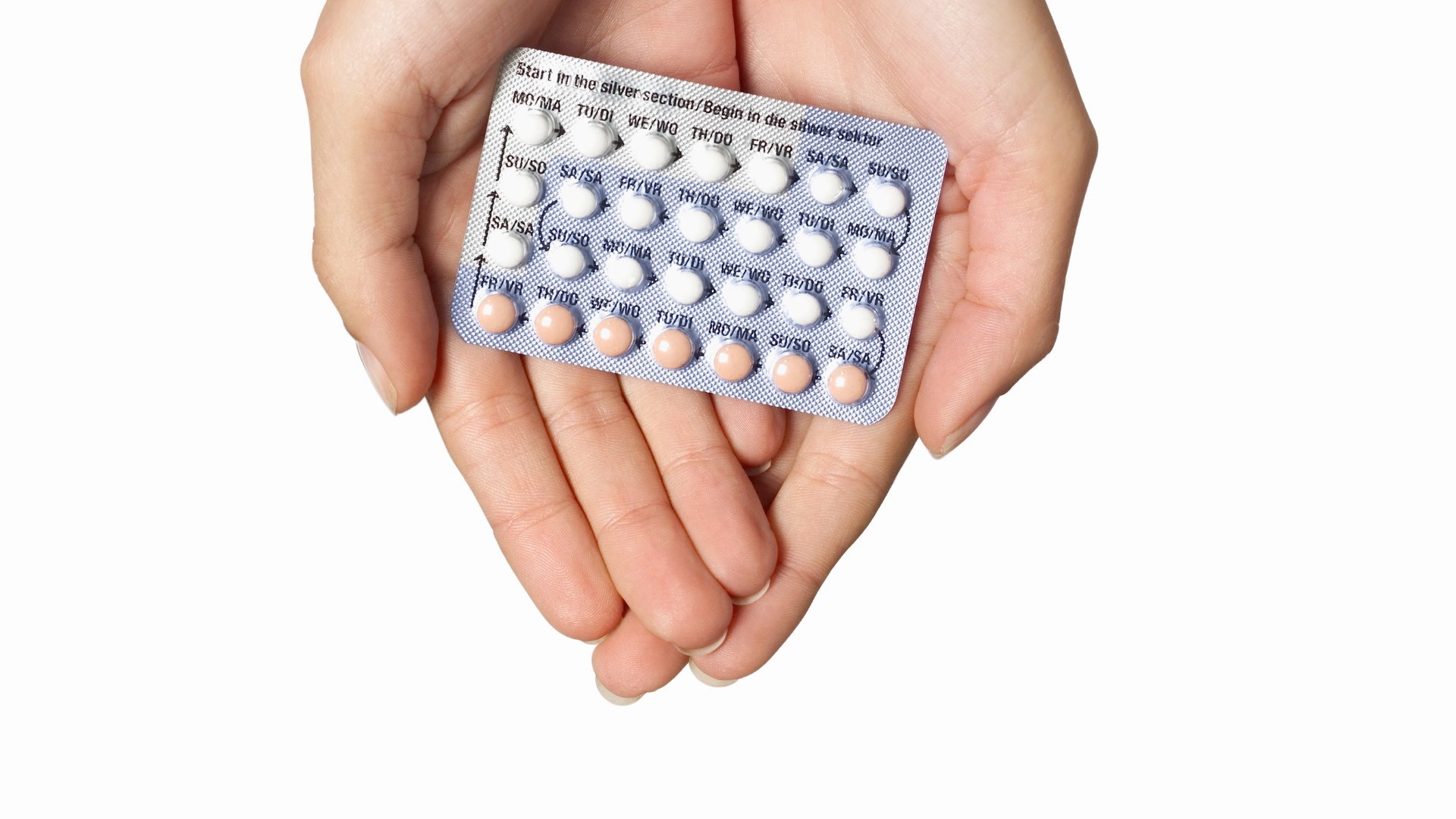
Today for #milkmonday we are highlighting a manuscript that was just published and brings to light an extremely important issue: can the type of contraception you use impact your milk supply? The answer we get from existing research is no, that for the average healthy mother who delivers a healthy, term infant, contraception does not impact milk supply. However, we see anecdotally that certain types of hormonal contraception can impact milk supply. So why is there a discrepancy, and what is the answer?
Depending on who is conducting the research and who is reading the study, what is considered clinically significant can vary.
We do this thing in research where we analyze the data with statistics to determine whether something we are witnessing is statistically significant. These statistics tell us whether the outcome we are seeing is happening by chance. Scientists and health professionals alike can use these numbers to inform a very black and white answer to something that may be much more complicated. As the authors of this manuscript put it:
For a woman who strongly desires to breastfeed, even a very small risk of iatrogenic lactation failure may be clinically relevant.
Bryant AG, Lyerly AD, DeVane-Johnson S, Kistler CE, and Steube AM. Hormonal contraception, breastfeeding and bedside advocacy: the case for patient-centered care. Contraception. 2019;99:73-76
You see, the studies that have been conducted may have observed a milk supply decrease some women, just not enough women to sway the statistics to be “significant”. As the article summarized nicely, someone with a public health interest in family planning may use this evidence to support placement of hormone-containing contraception. A lactation counselor, conversely, may use this evidence to support waiting to use hormone-containing contraception or advocacy for a non-hormonal contraceptive.
We then tie in the social injustices that surround reproductive health and breastfeeding, and the picture begins to get more complicated. It is unfortunate, but true, that poor women having children has a very different connotation than rich women having children. The same can be said for minority populations and women of color.
Health care providers have been shown to alter their counseling based on a patient’s race/ethnicity and perceived socioeconomic status.
Bryant AG, Lyerly AD, DeVane-Johnson S, Kistler CE, and Steube AM. Hormonal contraception, breastfeeding and bedside advocacy: the case for patient-centered care. Contraception. 2019;99:73-76
We know as health care providers, that counseling in a culturally competent and humble manner can help improve patient outcomes. However, when counseling shifts based on assumptions made off of race, ethnicity, or socioeconomic status, we are risk of widening the health disparities that exist.
The article closes by providing questions that can be used when counseling on breastfeeding and hormonal contraception, and it focuses on one thing: determining the desires of the patient through open-ended questions and providing recommendations based on PATIENT desires.
Health care provider recommendations should not be based on assumptions tied to race, ethnicity, socioeconomic status, sexuality, age, or any other factors. Recommendations should be evidence-based and tailored to the desires of the patients we are serving.
A 15-year old new mother who depends on WIC and SNAP benefits to provide for her new child should be given the same chance to breastfeed successfully as the 29-year old new mother who is financially independent. This includes avoiding hormonal contraception if the mother so chooses.

read more
Let’s talk about one of the scariest moments a parent can face. The baby has been fussy and seemingly unsatisfied after nursing. You make an appointment and the pediatrician informs you that you baby is losing weight. A rush of emotions and an overwhelming amount of questions pop into their head. Including a very important one: […]

read more
Around the holidays, I receive a flood of questions about how to safely enjoy an adult beverage while breastfeeding (and yes, you can have a drink!). The general rule: if it’s in your blood it’s in your milk. However, just because it goes into your milk does not mean it is there forever. The alcohol level in your milk maintains the same alcohol level as your blood. So once it is out of your blood it is also out of your milk. In fact, if you are responsible and plan your evening well, you may not even have to pump and dump your milk. Here are the tips I provide to new moms who are planning to have a drink while they are breastfeeding.
Breastfeed or pump right before you leave your baby, or if your baby is going with you, right before you decide to have a drink. This will help you avoid leaking or the need to pump due to fullness while your milk has alcohol in it.
Be prepared – have some pumped milk handy to feed if the baby gets hungry and your milk still has alcohol in it. If you are leaving the baby with a caregiver, leave the pumped milk with them and make sure they feel comfortable preparing and feeding a bottle. If this is your first time pumping, I recommend storing 3-4 ounces per milk bag and making bottles at a similar volume so that milk doesn’t have to be thrown away if the baby doesn’t eat it all. You can always feed more if the baby is still hungry.
Have your drink! Yep, I said it. It is perfectly acceptable to responsibly enjoy a drink or two while you’re breastfeeding. Research shows that it takes approximately 2 hours per drink for your body to filter all of the alcohol from your system. So if you consume 1 drink, you should wait a minimum of 2 hours from the time your finish your drink before breastfeeding. If you have two drinks, you should waits minimum of 4 hours after you finish the second drink to breastfeed. Every body is different, so if you feel intoxicated even if you have waited the “recommended” amount of time, you should not breastfeed your baby.
What if you feel full and need to breastfeed/pump? If you have waited the recommended amount of time after having a drink and you do not feel intoxicated, you can safely breastfeed or pump your milk and keep it to feed to your baby another time.
Follow your gut. At the end of the day I always tell mothers to trust their gut. If you are unsure about if you can breastfeed or keep pumped milk due to alcohol consumption, air on the side of caution. Feed a bottle of pumped milk or throw the pumped milk in question out.
*Please drink responsibly and make sure your child is appropriately cared for if choosing to enjoy a drink or two.
Update 3/7/2021: I felt that it was important to update this blog post to state this: if you have a drink (or two) and breastfeed your child simultaneously, the amount of alcohol that the infant will be exposed to is so small. Many parents choose to drink and not to “pump and dump” and for low amounts of alcohol intake, I do not believe this is dangerous.
Get Your copy →
Cross the finish line with confidence.
Don't walk into your IBCLC exam nervous - with our comprehensive study guide in your back pocket, you'll be prepared for every scenario and question.
